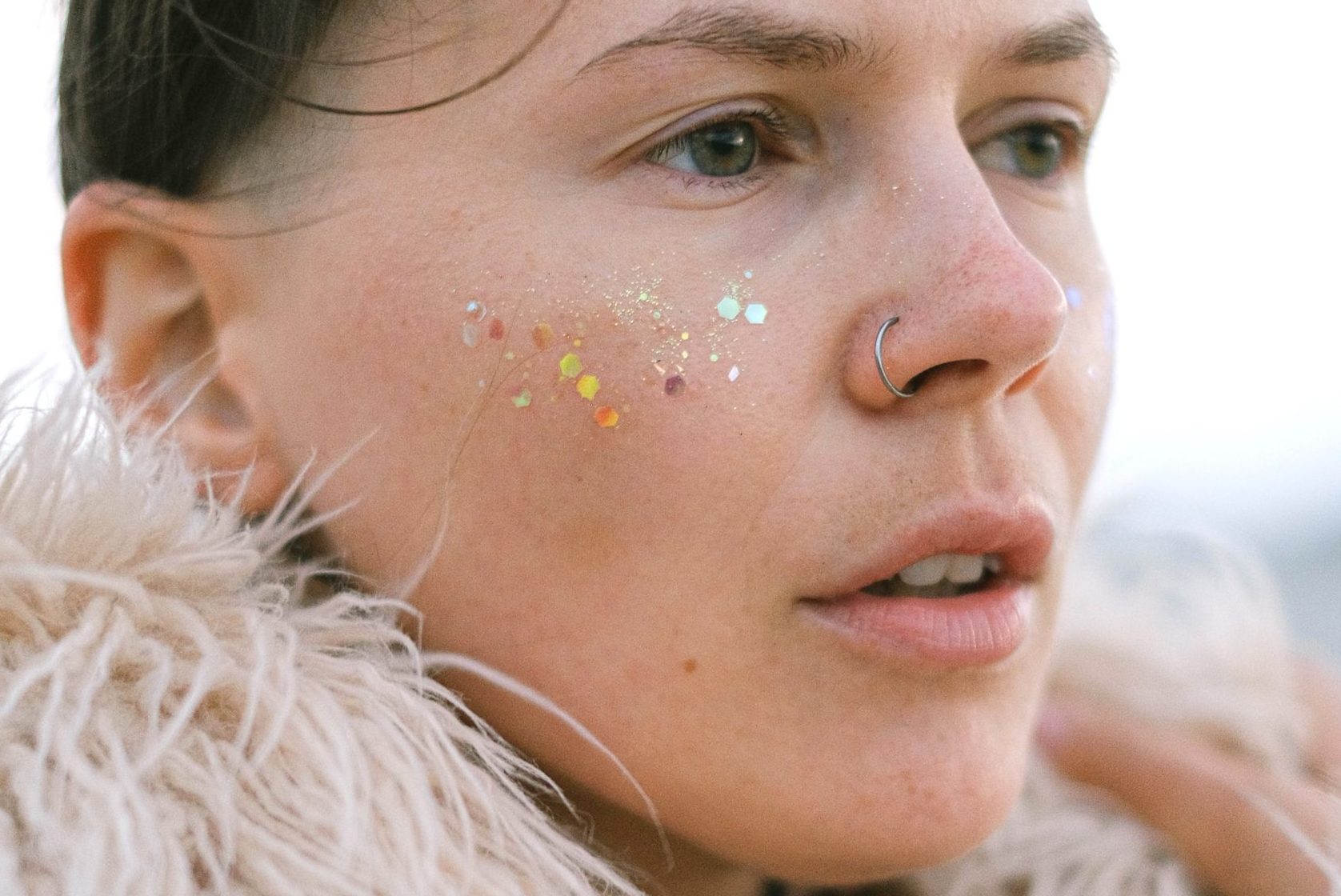Against the advice of dermatologists (and skincare articles) everywhere, pimple popping is practically a national pastime. Who hasn’t awoken to a pesky, juicy whitehead just begging to be squeezed? (Come on, hand emojis up.)
But when that one-off urge leads to regular zit- or skin-picking—or an occasional cuticle-pluck becomes a habit requiring Band-Aids—you might be dealing with a mental health issue called dermatillomania.
If you’ve never heard those seven syllables before—or the term excoriation disorder, as it’s also known—you may worry you’re the only one who picks their face, nails, arms, or ears until they bleed, and, in bad cases, even scar.
First, please know you’re not (see this Reel for proof). Dermatillomania affects 1.4 to 5.4 percent of the population, which is roughly 17 million people. And though excoriation disorder was just recently added to the DSM-5-TR, the guide of all mental health conditions, it’s been documented in medical literature as far back as the 19th century.
Picking your skin to the point of causing injury isn’t the only defining characteristic of excoriation disorder. “Another component of a skin picking disorder is the degree of distress and impairment that a person experiences in their life,” says psychologist Jen Viscusi, Psy.D., who specializes in obsessive-compulsive disorder (OCD), repetitive body behaviors (like dermatillomania), and PTSD.
“For example, often people feel embarrassment or shame related to skin picking,” she says, ‘so they avoid social situations [because of their resulting skin lesions], or they’re not able to go out and do important things without skin picking—even going to work.”
If your hand emojis are up again, we’re here to help. And that starts with knowledge.
Why In the World Do People Pick at Their Skin?
Scientists haven’t pinpointed one specific reason why someone develops dermatillomania. Potential causes trail on (and on) like the side effects fine print for an Rx med. Leading theories suggest it can result from trauma, illness, hormonal imbalance, emotional distress (including anxiety and depression), abuse, low self-esteem, or certain medications (like those used to treat ADHD). Some research also shows a link between skin picking and body dysmorphic disorder.
“There can be an underlying anxiety disorder, like obsessive-compulsive disorder,” explains psychodermatologist Amy Wechsler, M.D., who is board-certified in both dermatology and psychiatry and sees patients with skin-picking lesions, scarring, and acne.
While actively inflamed skin can prompt you to pick your face, say, it’s not always the reason. “There can just be anxiety or depression. It’s about finding where that compulsion [to pick your skin] comes from,” says Dr. Wechsler. In addition to treating the skin damage, she works to figure out if, and what, the psychological components are.
While Dr. Wechsler believes that most skin picking is related to some underlying issue, even if minor, excoriation disorder can stand alone. Sitting-around activities, like reading or watching TV, and simply feeling bored or tired can from time to time inspire the picking impulse.
GOTTA READ: Makeup That’s Safe for Picked Skin
“I can’t remember when I started,” says writer Sara Radin, who has been in therapy for several years to address her dermatillomania, as well as complex PTSD, depression, and anxiety (often a trigger for her skin picking). “I’ve just always done it. I bite my nails, pick my cuticles, and gnaw at any blemishes, bug bites, or scabs on my skin wherever they may be. I pick my skin multiple times a day—it’s a subconscious thing.”
In the past, Radin’s painful skin-picking—localized to her face, back, right arm, and chest—has led to skin infections that required a round of antibiotics. “I feel motivated to change the habit, but it’s really challenging to actually stop.”
How to Stop Skin Picking — Do You Need a Dermatologist or a Psychologist?
If you’ve decided to seek professional help, excellent first step! Despite what some might suggest, it’s not as simple as stopping cold turkey, particularly for people who aren’t even aware they’re picking their skin in the moment.
In those cases, it’s an automatic response to anxiety, stress, tension, or boredom, as opposed to focused repetitive behavior, which is a conscious response to these emotions or comes with a specific goal (like bursting that whitehead).
“There can be a real tactile component, so a lot of people will report touching their skin and when there are changes in texture, or they see dry skin, then they’re prompted to pick more,” says Dr. Viscusi. So the answer to that question above is: likely both.
A psychological evaluation can help map out the thoughts you have when you start to pick your skin or suddenly realize you’re mindlessly picking. And, since acne can often lead to repetitive skin picking, some pros prefer to get the breakouts under control first before addressing the behavior. “I’m going to aggressively treat the acne so I can get rid of anything, as fast as possible, that the person might pick at,” says Dr. Wechsler.
For over-the-counter products to help heal acne, Dr. Wechsler recommends Differin Gel, a popular adapalene (a type of retinoid) to speed up cell turnover, and salicylic acid, a beta hydroxy acid that fights excess oil within pores; try Jori Acne & Oil Control Primer. If flaky skin is your picking kryptonite, look for a moisturizer, like CeraVe Moisturizing Cream, that’s non-comedogenic, meaning it won’t clog pores and potentially exacerbate breakouts as it hydrates.
If the acne is more severe, Dr. Wechsler considers oral treatments. “Though there’s no overnight sensation,” she says, an Rx pill can work faster than topicals alone. This should not—we repeat: not—involve Accutane, which can cause serious skin damage to someone who picks.
No More Breakouts? What to Do Next to Stop Picking Your Skin
With underlying skin conditions like acne or eczema treated, it’s time to look at underlying urges. “I strongly suggest seeking help from a clinician who is really well-versed in OCD and body-focused repetitive behaviors,” says Dr. Viscusi, who often uses cognitive behavioral therapy (CBT) to treat excoriation.
CBT for skin picking, according to a study, “generally involves psychoeducation, cognitive restructuring, and an emphasis on relapse prevention through enhancement of self-efficacy, as well as agreement on clearly defined measures to prevent or address relapse.”
Sign up for our free newsletter
Legit tips and cool copes, delivered straight to your inbox.
By completing this form you are signing up to receive our emails and can unsubscribe anytime.
What this means in laywomen’s terms? Speaking with a therapist who specializes in excoriation disorder, changing negative thought patterns, and identifying and avoiding high-risk situations where you might be prompted to begin picking at your skin. Essentially, it’s habit reversal training.
“There is usually some overlap with habit reversal therapy, HRT,” says Dr. Viscusi. This may involve competing response training, where you replace skin picking (either as the urge to pick your skin hits or when you realize you’re doing it) with an alternative behavior.
“For example, if I’m sitting at my desk and tend to search for blemishes and pick my face, I might want to make sure I have something to occupy my hands, like clicking a pen or sitting on your hands,” she explains. In these situations, Radin pets her cat or plays with a stress ball.
Another helpful technique is creating a physical barrier between fingers and skin. Both experts recommend covering breakouts with a bandage or pimple patch, which is a little sticker that both covers and treats zits with salicylic acid; try Peach & Lily Acne Spot Dots. If your skin is raw and sore, look for plain hydrocolloid patches—no active ingredients. We like Hero Mighty Patch Invisible+ (which won a Best of Mental Health Award for this very purpose). Wearing gloves can curb the urge to pick too.

An unconventional, fashion-y alternative to wearing bandages over your picking finger: gorgeous rings with a gemstone at the tip (like the Best of Mental Health award-winning MAM Originals MakeUp 466 Midi Ring, below). They can serve as a discreet barrier, or as “a conversation starter for advocating and spreading awareness about skin picking,” says Lauren McKeaney, 31, a “silent-sufferer-turned-adamant advocate of dermatillomania” and founder of the Picking Me Foundation.
“When your hands are raising up to your fave spot to pick, you might catch the glimmer of the jewelry, and that sparkle will alert you to your hand going to ‘check on’ something,” McKeaney explains. “I do this as a strategy with black nail polish. It stands out and alerts me to where my fingers are.”
Dr. Viscusi has also had clients wear disposable silicone gloves in the shower (where many people can be tempted to pick since, you know, you’re naked), and the Picking Me Foundation suggests trying facial wipes, as they provide stimulation without direct finger-to-skin contact. Bioderma Sensibio H20 Wipes are gentle enough for sensitive or inflamed skin.
Radin relies on a few other tactics to prevent skin picking. “I’ve been tracking the behavior to increase my awareness of the habit through an app called Strides, and using ice to numb the sensation that makes me feel the need to pick.”
The Currents and The Leftovers
Sounds like a new dystopian Netflix series (wait, is it?), but what we’re talking about is how to treat right-now inflammation as well as the remnants of a bad pick. When skin is raw, reach for cleansers and moisturizers that do not contain fragrance or acids, which can be major irritants on skin with open wounds, says Dr. Wechsler.
Cetaphil Gentle Skin Cleanser is a classic liquid cream that gets the job done without soap, fragrance, sulfates, or foam (the latter itself, because of its texture, could provoke a picking urge). It’s also free of parabens, preservatives that, according to a study review in Skin Therapy Letter, are problematic on damaged skin.
For moisturizer, La Roche-Posay Cicaplast Balm B5 Soothing Therapeutic Multi-Purpose Cream is an excellent hydrator that also protects.
Skin majorly ouching? Consider a lotion with menthol and camphor. These ingredients tamp down pain and itch but also the sensation that can set off picking, says Dendy Engelman, M.D., associate clinical professor of dermatology at Albert Einstein College of Medicine in New York City, who likes Sarna External Analgesic Lotion.
Now to “the leftovers” part of our programming… In addition to addressing the cognitive component of her dermatillomania (say that five times fast!), Radin is now focusing on the residual scarring from previous picking. “Up until recently, I’ve been pretty lucky to have mostly clear skin,” she says. “Since I’ve been picking a lot lately, I am more concerned about scarring and have been exploring some solutions.”
For new or minor scars, Dr. Wechsler suggests over-the-counter silicone pads, like Elaimei Silicone Scar Sheets, which speed up wound healing, increase hydration, and promote collagen production. For larger or older scars, an in-office laser treatment, like VBeam or Fraxel, can help fade discoloration and remove scar tissue.
Radin, for her part, has narrowed her scar-minimizing routine to a mix of products—she’s still experimenting with application order—including Hero Rescue Balm, Mederma Scar Gel, Bio-Oil, Carter + Jane Postpick & PickFix, and Aquaphor.
“My dermatologist also just prescribed retinol, so I’ll be trying that as well,” Radin says. Like the Differin Gel mentioned above, an Rx retinol addresses both acne and rough skin texture.
Is It a Skin Picking Condition…Or Just a Bad Habit?
For people picking to the point of creating an open sore, trying to stop picking on their own but can’t, or the behavior really upsets them, it’s probably time to give therapy a go. But if your skin picking hasn’t reached clinical levels, Dr. Visuci says it’s okay to start on your own, building awareness around triggers.
You might start to notice things like, When my skin is dry, I tend to pick more, or When I have acne or eczema, I start to pick. Once you’re more cognizant of what’s going on, she says, you may be able to correct things just by being more mindful, keeping your hands away from your face, and maintaining a good skincare routine to minimize blemishes and dryness as much as possible.
No matter how mild or intense your skin-picking habit, the most important thing to remember is that you are not the only person struggling—far from it. “I never want [patients] to think they’re alone,” says Dr. Wechsler. “It’s not something that people often talk to other people about, even their close friends, so they often feel like [they’re] probably the only one doing this, and they’re definitely not. It’s very common and there’s always hope, and it’s absolutely treatable.”
It may not feel that way right now, and that’s understandable. And it may take years to finally break the habit. But creating a personalized treatment approach will set you on the right path. “I’m actively working on this, and I feel some sense of hopefulness that I’ll be able to stop with the help of my therapist and a self-care toolkit I can tap into whenever the urge arises,” says Radin.
If you’re comfortable, talking to others about your experience can itself be cathartic. In Radin’s case, “people have been incredibly supportive and helpful,” she says. “Sharing has helped me feel less ashamed and also made me feel like I’m connected to people I can relate to in a deeper way.”
READ NEXT: Best of Mental Health: Help Me Stop Picking
All products featured on Mental have been selected independently and editorially. When you buy from our links, we may earn a commission.
Geek Out on Our Sources
Jen Viscusi, Psy.D.: https://drviscusi.com/
Amy Wechsler, M.D.: https://www.dramywechsler.com/providers/amy-wechsler-m-d/
Skin Picking Stats: Grant J, et al. Skin Picking Disorder. The American Journal of Psychiatry. November 2012.
Excoriation Disorder Added to DSM-5-TR: Excoriation Disorder Workup. Medscape. August 22, 2022.
DSM-5-TR: DSM-5-TR Fact Sheets. American Psychiatric Association.
Causes of Skin Picking: Dermatillomania (Skin Picking). Cleveland Clinic. April 11, 2022.
Body Dysmorphic Disorder and Skin Picking: Grant JE, et al. Skin Picking Disorder With Co-Occuring Body Dysmorphic Disorder. Body Image. September 2015.
CBT for Dermatillomania: Lochner C, et al. Excoriation (Skin-Picking) Disorder: A Systematic Review of Treatment Options. Neuropsychiatric Disease and Treatment. July 14, 2017.
Competing Response Training: Heinicke M, et al. Reducing Risky Behavior with Habit Reversal: A Review of Behavioral Strategies to Reduce Habitual Hand‐to‐Head Behavior. Journal of Applied Behavior Analysis. July 20, 2020.
Facial Wipes for Cleansing: Skin Picking Prevention and Mitigation. Picking Me. July 19, 2018.
Silicone Gel for Wound Healing: Puri N, et al. The Efficacy of Silicone Gel for the Treatment of Hypertrophic Scars and Keloids. Journal of Cutaneous and Aesthetic Surgery. July-December 2009.
Parabens and Damaged Skin: Hafeez F, et al. An Overview of Parabens and Allergic Contact Dermatitis. Skin Therapy Letter. July-August 2013.